Consult for Septal Myectomy In Delhi/ HOCM Surgery In India
Dr. Sujay Shad, a leading heart surgeon, provides an effective HOCM surgery in India. To know about this surgery, it is important to know that HOCM is different from HCM, which is a type of non-obstructive hypertrophic cardiomyopathy.
HCM is a cardiac condition that occurs when the heart muscle is abnormally thick. A thickened heart muscle makes it difficult for the heart to perform its work, which functions to pump blood to the body. As a result, a number of HCM patients will notice shortness of breath. Some will get chest pain because the thickened muscle causes maldistribution of blood and nutrients to the heart muscle. A few patients will present with serious disturbances of the electrical system of the heart, causing what doctors call dysrhythmias; many of these are life-threatening.
Symptoms for HOCM
HOCM patients are the subset of HCM with obstruction to blood flow. Most patients with HOCM have no symptoms. Some patients complain of breathing difficulty or chest pain on exertion. Some patients have a history of lightheadedness or syncope. Unfortunately, the first presentation for many unlucky people may be a sudden cardiac death due to a sudden onset of disturbances in the heart’s electrical system.
- Chest pain, especially during exercise.
- Fainting, especially during or just after exercise.
- Shortness of breath, especially during exercise.
- Palpitations: Sensation of rapid, irregular, or forceful heartbeats.
- Hearing heart murmur sounds.
Diagnosis of HOCM Disorder
The prime diagnostic test is an echocardiogram. The doctor identifies the cause as well as the degree of obstruction to blood flow. When the obstruction is severe, we also make detailed notes about a surgical plan. On most occasions, the inlet valve for the left ventricle (mitral valve) is leaky.
An appropriate HOCM surgery in India performed by an expert cardiac surgeon relieves mitral valve leaks in over 90% of patients.
In addition, patients also undergo a cine MRI of the heart to aid in planning and document the risk of future dysrhythmias. A Holter test documents a continuous ECG recording for 24 hours for electrical disturbances.
Management of HOCM
This is a particularly challenging group of otherwise healthy young people whose life is at risk due to either ventricular arrhythmias or heart failure. For the last 50 years, many different means of treating these patients haven’t provided definitive and sustained results as compared to the newer surgical techniques.
Initial therapy consists of certain medications to slow the heart rate and allow more time for the heart to relax. However, if the patient’s symptoms continue or the degree of obstruction is severe, then surgery is recommended.
Surgery Options for HOCM
In our part of the world, an alternative and remarkably inferior strategy has been the mainstay of surgery to date. Here, while leaving the Septal abnormality in place, surgeons remove the mitral valve and replace it with an artificial mechanical valve to improve the obstruction. That does indeed remove the visible signs of obstruction but is a philosophically and practically inferior strategy. Parts of the mitral valve act as the skeleton of the heart, and that must be removed; this hurts cardiac function in the long term. Additionally, having a mechanical heart valve comes with its own complexities of managing blood thinners and their interactions with various drugs.
Extended Septal Myectomy:
Septal myectomy in Delhi, performed by Dr. Sujay Shad, is a newer procedure called extended septal myectomy that provides an excellent long-term result, and we have developed extensive expertise in this type of surgery.
The surgery is done via a standard sternotomy midline operation in the chest with standard heart-lung bypass.
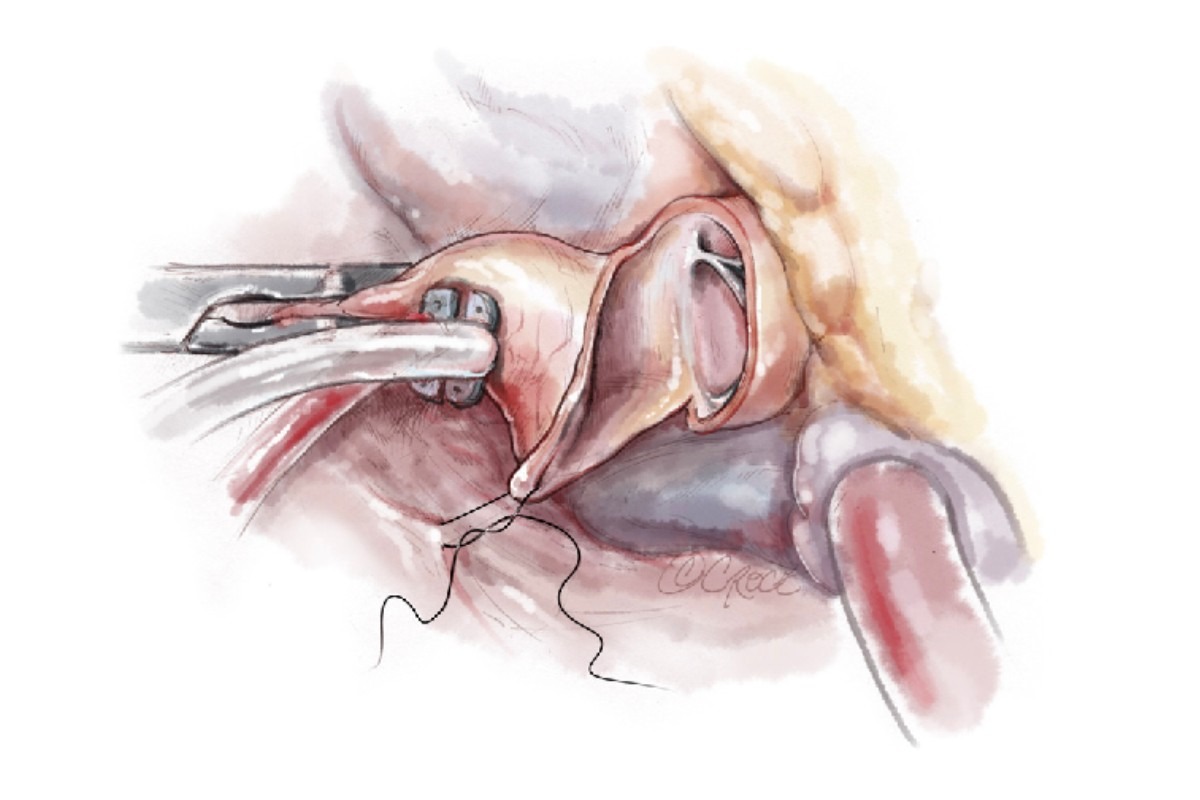
The heart is stopped for a short while, and we get to the bulge of the septum by making an opening in the aorta. The bulge is initially hidden from the surgeon by the patient’s aortic valve.
This is gently pushed away, and the septal bulge comes in view.
Now, based on the preoperative echo and MRI scans, a decision is already made about the length, width, and depth of the muscle to be removed. It is carefully removed in a step-by-step manner till I’m satisfied that the obstruction is relieved. After ascertaining satisfactory completion of resection and completing a final check, the aorta is closed, and slowly, the heart is allowed to start working. We make checks on the degree of obstruction at this stage, and if that is satisfactory, then the heart is given a full load of circulation, and the patient is separated from the heart-lung machine.
Further reading:
Dr. Eugene Braunwald initially defined HOCM. Dr. Barry Maron has invested his life in solving this difficult genetic pathology that affects young people and threatens their longevity. I would recommend all to visit the youtube channel that celebrates the work and life of this great master. http://youtu.be/CKlG7E4K3Qw.
I would also recommend for our readers the following link to see the views of Dr. Barry Maron, MD Director, Hypertrophic Cardiomyopathy Center Minneapolis Heart Institute Foundation Minneapolis MN: http://circ.ahajournals.org/content/116/2/196.full.pdf+html.
How to save your patient’s life?
You can read more and more about HOCM. I would request leading physicians and doctors to involve themselves with their patient’s care and directly pose questions to me about anything related to HOCM that you may feel important.
Together we can improve the lifestyles and lifespan of these high-risk young people.
Patients Concerns With Surgery:
Risk associated with surgery
Over the past 3 decades, HOCM surgery has become very efficient and safer. Today we have better instruments, better surgery and anesthesia techniques, better control of risk factors, and more efficient drugs. Septal myectomy in Delhi is one of the important surgeries performed by Dr. Sujay Shad. Statistically, patients who have undergone extended septal myectomy show excellent results up to and beyond 15 years after surgery.
The risk of this surgery is expected to be between 1-4% depending upon patient factors. In essence, this is a relatively safe operation.
Recurrence of Septal Bulge and HOCM
Once surgically removed to satisfaction, it is known to be curative. With no risk of recurrence. Some patients might require drugs to keep the heart rate slow. Some others might require drugs or Automatic implantable defibrillators (AICD) if their risk of ventricular dysrhythmias is high.
Risk of sudden death after surgery
The risk of sudden death in patients with HOCM is multifactorial. A host of factors come into play, and you can check your own risk of sudden death using HCM Risk-SCD | QxMD. If your risk of SCD prior to surgery is over 6% and AICD would generally be advised to mitigate any risk of the patient suffering ventricular fibrillation and death.
Pain After Surgery
All patients suffer pain after the surgery. This is well known for all types of operations.
The truth is that chest surgery causes slightly less pain than a belly operation. Pain will make a patient eat less, walk less, talk less, exercise less, sleepless, and in short, one can also become depressed. And I know this very well by closely observing patients over 35 years.
I insist that my patient should not suffer pain after surgery. A pain-free patient (or nearly pain-free patient) is more active from early after surgery and fully enjoying life. Since they start behaving and exercising normally very soon after, they don’t suffer complications of inactivity.
Recovery and rehabilitation after surgery
These follow a normal pattern of recovery as after any open chest procedure, and most patients are discharged within 4-8 days after surgery. A special issue with HOCM patients in the period after surgery is the stability of ECG rhythm. We keep a close watch on the patient’s ECG for 5-7 days after surgery and sometimes need to use drugs / temporary or permanent pacemakers to control rhythm disturbances.
- First 2 days
All patients are cared for in an intensive care unit for the first two days after surgery. A dedicated specialist cardiac surgery postop care nurse is with the patient 24×7. Monitoring each and every vital parameter and looking after Pulse, BP, variety of pressures from within the heart chambers, lung function whether the patient is breathing by a machine or by themselves. Kidney, liver, brain functions, need for blood transfusion and intravenous fluids, etc., are also checked. There is a dedicated Cardiac Surgery and a Cardiac Anesthesia Doctor in the hospital only for Cardiac Surgery patients to supervise the nurses. I am also available around the clock for any issues for which doctors or nurses might seek advice.
- Next 3-5 days
Most patients start to walk to the bathroom before this stage, food progressively becomes more interesting, and they are shifted to the SICU or ward depending upon many clinical factors. While nurses and doctors are always around, this time is spent making patients more and more independent for their daily needs.
- Day of discharge
The patient and their relatives are educated in a rehabilitation class by a rehabilitation expert. All patients learn to get in and out of bed unsupported. Patients are expected to travel home by car, sitting in the front seat with a towel between the chest and seat belt. All patients are asked to climb stairs and not be carried in chairs as makeshift palanquin.
Bathing as suggested by doctors and nurses onwards. Exercises as per the embedded video. (once we make the video link here)
- First Review after a week
Some blood tests and ECG and CXR are required at this clinic attendance. Most patients can start short walks in the local parks and increase exercise.
- A month after surgery
Most self-employed people who can control their timings are back to work by this time; people in employment need about 2 months to regain strength.
To know about Septal Myectomy surgery in Delhi, please feel free to contact us.


